- Blog
- Trifox frame
- Hyperkalemia ecg findings
- Rekord buddy virtual dj
- The sun origin secret code
- Php for loop
- Rightfont adobe plugin
- Image bucket of corona
- Factorio lane balancer
- Bus driver riddle
- Supreme commander 2 hidden objectives
- Osprey aether
- The lost masterpiece
- Pixlr web editor
- Top best free porn sites
- Miami weather live cam
- Getamped2 skin contest 2012
- A visit to friends chekhov
- Purchasing adobe edge animate cc
- The simpsons larry the looter
- Hotel cubo in ljubljana
- Imyfone ios system recovery thepiratebay
- Quickshot launch video
- Ifttt nasa picture of the day not working
- Sonarr mass rename
- Deck tiles
- App like boxer for mac
- Download computer cuisine deluxe 7-0-app mac
- Blog
- Trifox frame
- Hyperkalemia ecg findings
- Rekord buddy virtual dj
- The sun origin secret code
- Php for loop
- Rightfont adobe plugin
- Image bucket of corona
- Factorio lane balancer
- Bus driver riddle
- Supreme commander 2 hidden objectives
- Osprey aether
- The lost masterpiece
- Pixlr web editor
- Top best free porn sites
- Miami weather live cam
- Getamped2 skin contest 2012
- A visit to friends chekhov
- Purchasing adobe edge animate cc
- The simpsons larry the looter
- Hotel cubo in ljubljana
- Imyfone ios system recovery thepiratebay
- Quickshot launch video
- Ifttt nasa picture of the day not working
- Sonarr mass rename
- Deck tiles
- App like boxer for mac
- Download computer cuisine deluxe 7-0-app mac
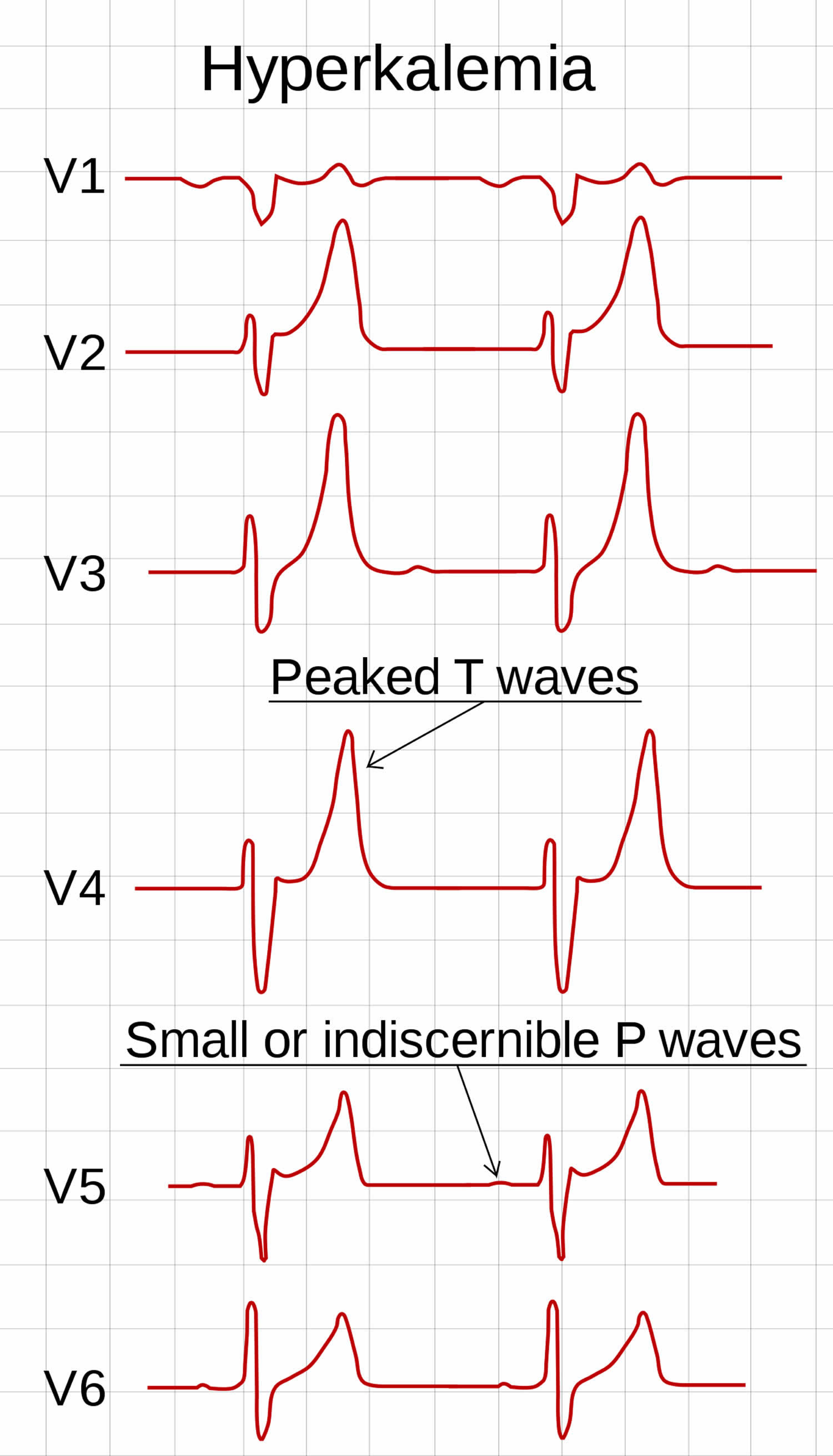
Hypomagnesemia is often times associated with hypokalemia thus it is important to check a magnesium level in any patient who presents with arrhythmia. Hypokalemia can occur secondary to medications (common culprits include hydrochlorothiazide and furosemide), gastrointestinal loss, overzealous treatment for hyperkalemia or shifting of potassium into the cell. Potassium levels that are critically low (<1.7) can lead to torsades de pointes. Hypokalemia causes enlarged and prominent T waves on the EKG. The U-wave is a deflection following the T wave. EKG changes can include increased amplitude and width of P wave, T wave flattening and inversion, prominent U waves and apparent long QT intervals due to merging of the T and U wave. Similar to elevated potassium levels, low potassium levels can cause myocardial arrhythmias and significant ectopy. Hypokalemia is defined as a potassium level less than 3.5, but EKG changes generally do not occur until the level goes below 2.7. The EKG can also provide early indication of a low potassium level. After the potassium level has been resulted additional treatment to aid in shifting the potassium intracellularly and aiding total body excretion. The calcium will stabilize the cardiac membranes and in turn prevent further arrhythmias from developing. Some emergency medicine practitioners advocate for calcium administration with peaked T-waves alone, while others will only treat if additional findings are seen. The most important initial treatment that should be administered if EKG changes are seen is administration of calcium gluconate or calcium chloride. Note how the PR and QRS lengthen in hyperkalemia until the patient develops a “sine-wave” pattern EKG For example, peaked T waves might correspond with a potassium level of approximately 6, whereas cardiac arrest generally occurs at higher levels. These progressive changes can correlate with rising potassium levels. EKG changes progress from peaked T-waves to widened QRS and eventually to ventricular tachycardia, fibrillation or pulseless electrical activity arrest. Patients who are high risk include those on renal replacement therapy(peritoneal or hemo-dialysis), those with concern for diabetic ketoacidosis or patients with acute renal failure. Performing an early EKG, especially in high-risk patients, paying careful attention to changes consistent with hyperkalemia can be life saving. Note the peaked T-waves in this patient with a potassium of 7.0 When there is excess extracellular potassium, either from shifts or inability to excrete, patients can experience arrhythmias and potentially cardiac arrest. It is important to recall that potassium is a primarily intracellular cation. In order to reduce morbidity and mortality associated with this condition, early identification and treatment is key.

Hyperkalemia is defined as a serum K of greater than 5.5. To discuss common etiologies and clinical presentation of each of the above named electrolyte abnormalitiesĮlevated potassium level is a common and life threatening condition that is seen in the emergency department.To identify EKG changes associated with hyper- and hypocalcemia.To identify EKG changes associated with hyper- and hypokalemia.A combination of clinical history paired with EKG findings consistent with elevated potassium levels, should prompt emergent treatment to stabilize the cardiac membrane. This EKG can be used to evaluate for ischemic changes, but also can give the provider some early insight into the patient’s electrolyte levels. SAEMF/CDEM Innovations in Undergraduate Emergency Medicine Education GrantĬareer Development and Mentorship CommitteeĬommunications and Social Media CommitteeĪn electrocardiogram(EKG) is often times obtained on patients shortly after they arrive in the emergency department. Presidential Address: Where Do We Go From Here?ĮMF/SAEMF Medical Student Research Training Grant
Virtual Rotation and Educational ResourcesĬommittee Update: NBME EM Advanced Clinical Examination Task Force Visit us on Twitter LinkedIn Facebook YouTubeĮffective Consultation in Emergency Medicine Video
